No one likes ads. We know that. But without ads this site simply could not exist. Please be fair to us and others and consider turning them on.
Thanks for any assistance.
by bohica » 17 Mar 2014, 16:54
There are no such «Bulges» on the Wing Root panel
by exfltsafety » 18 Mar 2014, 04:22
by fasteagle » 18 Mar 2014, 06:53
by tbarlow » 18 Mar 2014, 16:26
by hoghandler » 21 Mar 2014, 13:12
All the panels that we build have those bulges on them. There are two per panel and they are stamped into the skin panel. If I could, I would post a pic of them but they wont let us take pics at the factory.
I do believe it has some thing to do with the wing attach fittings.
by zen4130 » 08 Jan 2023, 13:58
Hi folks, dug this one up from the dead for the same reason as the OP. Does anyone have any more info regarding these bulges? Can anyone confirm they’re because of wing attachment fittings or is it something else? Thanks
- Learning Objectives
- Importance of Radiography in Endodontics
- Diagnosis
- Identifying Pathosis
- Determining Root and Pulpal Anatomy
- Characterizing Normal Structures
- Treatment
- Determining Working Lengths
- Moving Superimposed Structures
- Locating Canals
- Differentiating Canals and Periodontal Ligament Spaces
- Evaluating Obturation
- Follow-up Evaluation (Recall)
- Identifying New Pathosis
- Evaluating Healing
- Special Applications
- Working Radiographs
- Radiographic Sequence
- Diagnostic Radiographs
- Angulation
- Master Cone
- Other Considerations
- Exposure Considerations
- Cone-Image Shift
- Principles
- Faciolingual Determination
- SLOB Rule
- Prologue
- Introduction
- Radiation Biology
- Equipment for 2D Image Capture
- Handheld Units
- Intraoral Image Receptors
- Types of Digital Image Receptors
- Photostimulable Phosphor Plates
- Solid-State (Direct) Sensors
- Dental Film
- Techniques for Intraoral Image Capture
- Tube Shift
- Endodontic Imaging Needs
Learning Objectives
After reading this chapter, the student should be able to:
We are sick of the roentgen ray . . .you can see other people’s bones with the naked eye, and also see through eight inches of solid wood. On the revolting indecency of this there is no need to dwell. But what we seriously put before the attention of the Government . . .that it will call for legislative restriction of the severest kind. Perhaps the best thing would be for all civilized nations to combine to burn all works on the roentgen rays, to execute all the discoverers, and to corner all the tungstate in the world and whelm it in the middle of the ocean. Editorial in the Pall Mall Gazette, London, 1896
Obviously (and fortunately), the concern expressed by the editorial in this London publication did not become the popular view of radiography. Radiographs are essential; they are a second set of “eyes” for the dentist. This is particularly true in endodontics, in which so many diagnostic and treatment decisions are based on radiographic findings. Because most structures of concern are not visible to the naked eye, there is considerable dependence on radiographs, which are an obvious necessity and a blessing. But they also may be somewhat of a liability from the standpoint of both safety and time, and unfortunately, radiographs are often overinterpreted or underinterpreted.
A radiographic exposure is an irreversible procedure; therefore, only necessary exposures should be made. With the increasing emphasis and justifiable concern for radiation safety, overall radiation exposure must be minimized. However, the radiation dosage to oral and other tissues has been calculated to be very low and to cause minimal (but some) risk.
Another concern is the time required to make and process individual radiographs—time is money. Therefore, in the interests of both safety and time, only the radiographs necessitated by the procedure should be made.
This chapter discusses radiography as applied to endodontic procedures. Radiography as a discipline in dentistry has become increasingly important with advances in technology and has recently been granted specialty status, thereby replacing endodontics as the youngest dental specialty. Technology has exploded in recent years, with new devices and approaches that require special training and experience. How these new devices and approaches apply to diagnosis and treatment in endodontics is discussed later in this chapter.
Importance of Radiography in Endodontics
The use of digital radiography is becoming more common in dentistry. Although there are technical advantages over conventional approaches, the same limitations apply. Overall, digital radiographs are equivalent to conventional radiographs with regard to diagnostic and treatment-related accuracy. These factors and other considerations are discussed further throughout this chapter.
Diagnosis
Diagnostic radiology involves not only identifying the presence and nature of pathosis, but also determining root and pulp anatomy and characterizing and differentiating other normal structures.
Identifying Pathosis
Radiographs must be studied carefully by someone with a working knowledge of the changes that indicate pulpal, periapical, periodontal, or other bony lesions. Many changes are obvious, but some are subtle.
Determining Root and Pulpal Anatomy
Determining the anatomy involves not only identifying and counting the roots and canals, but also identifying unusual tooth anatomy, such as dens invaginatus and a C -shaped configuration, and determining curvatures, canal relationships, and canal location. Identification also includes characterizing the cross-sectional anatomy of individual roots and canals ( Fig. 12.1 ).
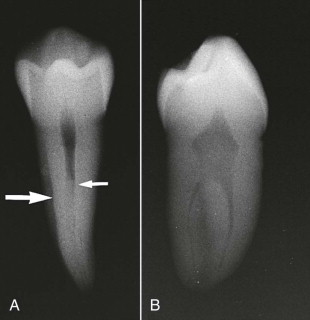
A, The facial projection of this premolar gives some limited information about pulp/root morphology. “Fast break” (small arrow) usually indicates canal bifurcation. A double root prominence on the mesial surface (large arrow) indicates two bulges and a concavity; its absence on the distal surface indicates a flat or convex root surface. B, The same premolar from the proximal view. The presence of two definitive canals, each in its own “root bulge,” is confirmed.
Characterizing Normal Structures
Numerous radiolucent and radiopaque structures often lie in close proximity. Frequently, these structures are superimposed over and obscure crowns and roots. These must be distinguished and differentiated from pathosis and from normal dental structures.
Treatment
“Working” radiographs are made while the dental dam is in place, which creates problems in film placement and cone positioning. These radiographs are exposed during the treatment phase and have special applications.
Determining Working Lengths
The distance from a reference point to the radiographic apex is determined precisely. This establishes the distance from the apex at which the canal is to be prepared and obturated.
Moving Superimposed Structures
Radiopaque anatomic structures often overlie and obscure roots and apices. Using special cone angulations, these radiopaque structures can be “moved” to give a clear image of the apex.
Locating Canals
Canal location is obviously essential to success. Standard and special techniques allow the practitioner to determine the position of canals not located during access.
Differentiating Canals and Periodontal Ligament Spaces
Canals end in the chamber and at the apex. A periodontal ligament space ends on a surface and in a furcation (molars) and demonstrates an adjacent lamina dura ( Fig. 12.2 ).
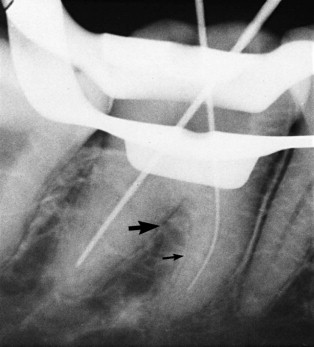
Evaluating Obturation
Postoperative radiographs provide considerable information on canal preparation and obturation. The length from the apex, density, taper, preservation of original canal shape, and general quality of obturation in each canal are determined from these radiographs.
Follow-up Evaluation (Recall)
Ultimate success is verified at specified intervals of months or years after treatment. Because failures often occur without signs or symptoms, radiographs are essential to evaluate periapical status.
Identifying New Pathosis
The presence and nature of lesions that arise after treatment are best detected on radiographs. These lesions may be periapical, periodontal, or nonendodontic. It is important to remember that such lesions frequently present with no overt signs or symptoms and are detectable only on radiographs ( Fig. 12.3 ).
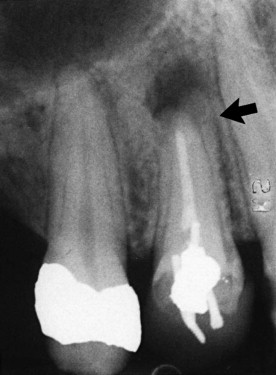
Failed root canal treatment because of missed root or canal. This mesial-angled radiograph clearly shows the untreated lingual root (arrow).
(Courtesy Dr. L. Wilcox.)
Evaluating Healing
Pretreatment lesions should be resolving or should have resolved. In a successful (healed) treatment, restitution of generally normal structures should be evident on recall radiographs ( Fig. 12.4 ).
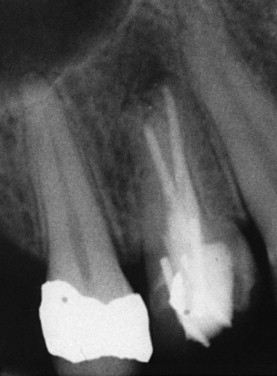
Same tooth as shown in Fig. 12.3 . Recall radiograph after 9 months shows almost complete regeneration of bone, indicating a healing lesion. A permanent restoration must be placed as soon as possible.
Special Applications
Varying either the vertical or, particularly, the horizontal cone angulation from parallel alters images and enhances interpretation. These shifts reveal the third dimension and superimposed structures. Shifts also permit identification and positioning of objects that lie in the faciolingual plane.
Working Radiographs
Working radiographs are essential aids to treatment and are exposed when necessary but with discretion.
Radiographic Sequence
Radiographs are made in a recommended order and number for each procedure. The minimum number is described here, although special situations may require additional exposures.
Diagnostic Radiographs
The number of exposures depends on the situation. For diagnosis in most cases, only a single exposure is necessary. A properly positioned film and cone (usually a parallel projection is best) permits visualization at least 3 to 4 mm beyond the apex. The initial diagnostic radiograph is used primarily to detect pathosis and to provide general information on root and pulp anatomy. A bitewing radiograph may aid in determining the extent of caries or in detecting caries or an open margin of a crown. Usually, it is not necessary at this time to make additional films for identification of additional canals except in endodontically treated teeth, in which missed canals can be identified by using a shift.
If other films are at hand, each gives a slightly different view of the same tooth ( Fig. 12.5 ). Examine the tooth on each film in which it appears.
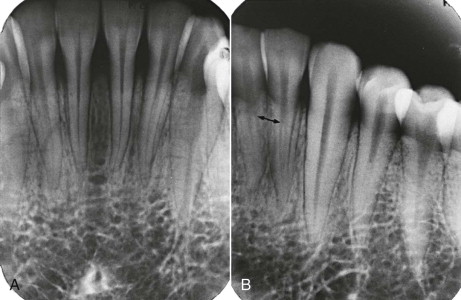
A, Facial projection of incisors suggests a single canal and a single root. B, Distal (canine) projection gives a different perspective. The canals of the lateral and central incisors are seen to bifurcate in the middle third of the root (arrow) and reunite in the apical third.
Angulation
Unquestionably, the most accurate radiographs are made using a paralleling technique. The advantages are (1) less distortion and more clarity and (2) reproducibility of film and cone placement with preliminary and subsequent radiographs. Reproducibility is important when assessing whether changes occurring in the periapex indicate healing or nonhealing. Paralleling devices enhance reproducibility.
There may be special situations in which the paralleling technique is not feasible, such as a low palatal vault, maxillary tori, exceptionally long roots, or an uncooperative or gagging patient; these circumstances may necessitate an alternative technique. A second choice is the modified paralleling technique; the least accurate technique is the bisecting angle.
These radiographs are usually neither parallel nor bisecting angle. The technique used is called modified paralleling. Essentially, the film is not parallel to the tooth, but the central beam is oriented at right angles to the film surface. In endodontic working radiographs, a further modification is made by varying the horizontal cone angle. Specific details of film/sensor and cone placement and radiographic interpretation are discussed later in this chapter.
In general, establishment of working length should require only a single exposure. If a root contains or may contain two superimposed canals, either a mesial or distal angle projection is absolutely necessary; the straight facial view is not particularly helpful. Additional working length radiographs may be required later for confirmation of working lengths to detect the presence or lengths of newly discovered canals ( Fig. 12.6 ) or for reexposure if an apex has been cut off in the first radiograph.
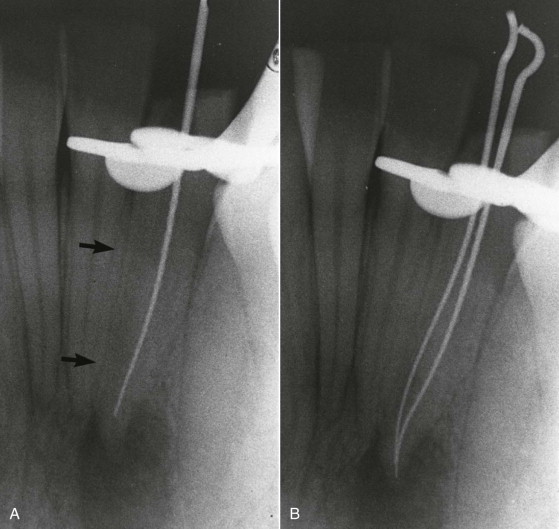
Identifying and locating a canal. This incisor was rotated, requiring mesially angled working radiographs. A, The file is off-center, as indicated by the mesial root surface (arrows) . Therefore, the file is in the facial canal. B, A search to the lingual locates the lingual canal. There is a common canal apically.
Master Cone
The same principles used with working length films apply. With proper technique, only one radiograph is necessary to evaluate the length of the master gutta-percha cone. The master cones should extend to, or very close to, the corrected working length. (Procedures for the fitting of master cones are discussed in Chapter 18 .)
Other Considerations
Additional working radiographs are often required. For example, they are useful as aids in locating a canal or in determining the occurrence of procedural accidents (perforations, separated instruments, or ledges). Variations in cone positioning and angulation are made as required. When there is doubt about the accuracy of the master cone fit, an intermediary fill radiograph may be exposed after the master cone has been condensed with sealer but before the obturation is finalized. Errors in length or density can be corrected at this stage.
The same basic principles used for diagnostic radiographs apply. At least a parallel projection should be made. In teeth with multiple canals, it is desirable to supplement this with an angled projection to visualize separate superimposed canals for separate evaluation of each. However, the radiograph gives only a rough indication of obturation length and quality.
The same principles used for diagnostic and obturation radiographs (parallel projection and exposure factors) apply to recall radiographs. There is one exception. If treatment is deemed to be questionable or a failure, additional angled radiographs are often required to search for a previously undetected canal or other abnormality.
Exposure Considerations
Proper x-ray machine settings and careful film processing are important for maximal quality and interpretative diagnostic and working radiographs. D film (Ultraspeed) and E film (Ektaspeed) have been used and compared. Although D film has been shown to have slightly better contrast, overall suitability is equivalent for the two film types. The newer Ektaspeed Plus film produces an image similar in quality to Ultraspeed film but requires only half the radiation of Ultraspeed.
The optimal setting for maximal contrast between radiopaque and radiolucent structures is 70 kV. Exposure time and milliamperage should be set individually on each machine. Therefore, the preferred film types are E and Ektaspeed Plus to minimize x-ray irradiation at 70 kV and to maximize clarity.
Digital radiographs require much less exposure time than conventional radiographs, which is a definite advantage. In general, there does not appear to be a significant difference in clinical accuracy between conventional and digital radiography or among different digital radiography systems.
Cone-Image Shift
The cone-image shift reveals the third dimension.
Principles
The cone-image shift technique separates and identifies the facial and lingual structures. An example is the mesiobuccal root of a maxillary molar that contains two superimposed canals. The cone shift separates and permits visualization of both canals.
Faciolingual Determination
Principles of relative movement of structures and film orientation are applied to the differentiation of object position ( Figs. 12.7 and 12.8 ).
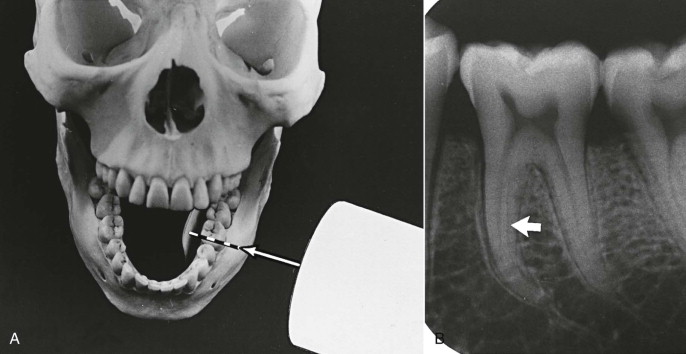
A, The film is positioned parallel to the plane of the arch. The cone has the central ray (arrow) directed toward the film at right angles. This is the basic cone-film relationship used for horizontal or vertical angulations. B, There is a clear outline of the first molar but limited information about superimposed structures (canals that lie in the buccolingual plane). The arrow points to a periodontal ligament space adjacent to a superimposed root bulge, not to a second canal.
(From Walton R: Endodontic radiographic techniques, Dent Radiogr Photogr 46:51, 1973.)
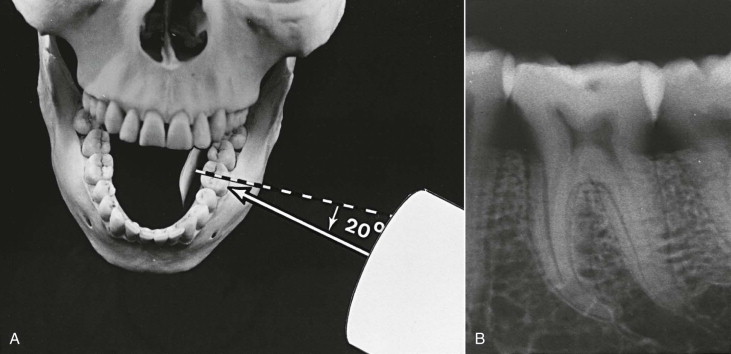
A, The horizontal angulation of the cone is 20-degrees mesial from the parallel, right-angle position (mesial projection). B, The resultant radiograph demonstrates the morphologic features of the root or canal in the third dimension. For example, two canals are now visible in the distal root of the first molar.
SLOB Rule
When two objects and the film or sensor are in a fixed position buccal and lingual from each other, and the radiation source (cone) is moved in a horizontal or vertical direction, images of the two objects move in the opposite direction ( Fig. 12.9 ). The facial (buccal) object shifts farthest away; the lingual object moves in the direction of the cone movement. The resulting radiograph shows a lingual object that moved relatively in the same direction as the cone and a buccal object that moved in the opposite direction. This principle is the origin of the acronym SLOB (same lingual, opposite buccal).
Only gold members can continue reading. Log In or Register to continue
Prologue
Dr. William Herbert Rollins was already an established Harvard-trained physician and dentist when x-rays were discovered in 1895. Dr. Rollins, like his contemporaries, was fascinated by the usefulness of x-ray images. However, he was also one of the first to recognize the poorly understood―but genuine―risks associated with x-ray imaging.
Suffering radiation erythema to his hand in January 1898, and having seen the lethal effects of x-rays in his guinea pig experiments, Rollins attempted to caution his contemporaries of its dangers; however, the enthusiasm for the new x-ray technology was blinding radiographers to its morbid hazards. By the late 1920s, it was clear that there were biorisks associated with x-rays as the ranks of prominent radiographers in the New England area had been thinned. Further demonstrating this risk was the fact that at radiology meetings in the 1920s, roast beef was rarely served because the radiographers wore gloves to hide their scars and, by doing so, could not cut the roast beef with the cutlery provided.
It was not until the post-World War II atomic era, that the scientific community again began to heed the warnings of Rollins from a half century earlier.
Introduction
By virtue of its ability to image beyond the scope of the intraoral examination, radiography is an indispensable part of the diagnostic process in dentistry. Within this scope of oral health care, endodontics makes full use of this most useful of diagnostic techniques.
Imaging in the 21st century no longer relies solely on the use of x-rays for diagnostic imaging. Other imaging modalities from which dental care now benefits include optical scan imaging, magnetic resonance imaging, and on the frontier, ultrasound imaging. , However, with the advent of digital technology, x-ray imaging remains progressive with constant innovation. These innovations keep x-ray imaging an integral and up-to-date part of the diagnostic process for endodontic care.
The use of sensors in dental imaging has changed dramatically, from the earliest days of photographic emulsion on glass plates, to the development of plastics to support radiographic emulsion (i.e., film). In the 1980s, intraoral digital sensors were introduced by Dr. Frances Mouyen. Endodontics eventually embraced this technology because digital sensors dramatically facilitated the efficiency at which endodontic procedures could be completed.
In the 1960s endodontics became the eighth recognized dental specialty of the American Dental Association. At the same time, extraoral panoramic imaging became the exhilaration of dentistry with its ability to image large areas of the jaws in a single exposure. However, extraoral imaging was not as beneficial to the intricacies of endodontic patient care until the introduction of cone beam computed tomography (CBCT). In the 21st century, CBCT is a digital extraoral imaging modality that has greatly facilitated endodontic care. This chapter outlines the utility of radiographic imaging for endodontic patient care with the continued use of intraoral radiography as well as the progressive advances initiated with extraoral CBCT.
Radiation Biology
Contemporary clinicians must still deal with the reality that there are long-term risks that may be realized from exposure to x-radiation. Endodontic care will typically lead to multiple patient x-ray exposures. The radiation dosage to oral and other tissues has been calculated to be very low and extrapolated to cause minimal (but some) risk. , Table 3.1 illustrates the effective doses of various dental imaging procedures. This table provides the reader with a measure of the biorisk from intraoral exposures in relation to other dental imaging procedures. A more detailed radiation dosimetry review is available elsewhere. ,
Differential Diagnosis for the Most Common Injuries to the Periodontium
In pediatric patients, the biorisks from the x-radiation are greater than the adult risks for a given radiation dose. This increased risk is due to the pediatric patient’s inherently greater radiosensitivity and because children have more remaining years of life during which a radiation-induced malignant neoplasm could develop. Hence, as with any imaging modality, the decision to use any diagnostic x-radiation is an objective-laden thought process where the benefits of the information obtained must outweigh the risks of the x-radiation.
Equipment for 2D Image Capture
Dental x-ray units have changed very little over the years since David Coolidge designed the first enclosed x-ray tube and tube head, the Victor CDX, in 1919.
Exposure times have decreased to less than 20% of the exposures from as little as three decades ago. Because of this, the need for large x-ray tube heads housing the larger generators needed to produce kV potentials greater that 70 kV has decreased. The need for high milliamperage (i.e., mA settings greater that 10 mA) is also no longer indicated with the shorter exposure times needed for digital receptors. Most contemporary x-ray tube heads are smaller with kV potentials between 60 and 70 kV and mA in the 6- to 8-mA range. With some exposure times now less than 0.10 seconds, most units have digital microprocessor timers that can reproducibly generate direct current (DC) exposures in the 0.05- to 0.10-second range. These smaller x-ray units produce adequate x-radiation to expose contemporary digital receptors, including American National Standards Institute (ANSI) F speed film, and reduce patient radiation dose with the shorter exposure times
Another option available in dental x-ray units is the recessed x-ray tube. Instead of the x-ray tube placed adjacent to the window within the tube head and the position indicating device (PID), contemporary x-ray tube heads have the x-ray tube recessed further away from the window ( Fig. 3.1 ). The recessed tube produces a longer focal distance (x-ray source-to-object distance), which projects a sharper image outline. With an increased focal distance, the inverse square law dictates that the exposure must be increased. However, even though the exposure needs to be greater to obtain a diagnostic image density, the patient dose is actually decreased, which is an added benefit of the recessed x-ray tube. This benefit is because the increased distance will prevent many of the low-energy x-ray photons in the beam from reaching the patient. Thus the recessed x-ray tube acts as a distance filter, which will decrease the patient dose.

X-ray tube head with position dot indicating the position of the focal spot that is inside the x-ray tube head (red arrow) . The inset image demonstrates the increased length of the focal distance. This increased length offers sharper image outlines and reduced patient dose.
Handheld Units
In the past decade, handheld x-ray units for dental imaging have become very popular in clinical practice. ,
Handheld units were originally designed for the benefit of mobility to provide dental imaging in remote locations where standard equipment is not available or for nonambulatory patients in need of dental services who cannot access standard dental facilities. Because these units are made for portability, they have become more popular in regular office designs and are used as a single unit for multiple standard operatories. Image quality is generally acceptable; however, due to the portability, the maximum kV and mA are less than those possible with standard units. The biggest issue with handheld units is the radiation dose to the operator if used without proper training. However, units have been shown to have adequate shielding to protect the operator if used properly with a backscatter shield.
Proper usage includes assuring that backscatter shields are attached to the units so that the operators can keep their bodies within the protective range of the shield ( Fig. 3.2 ).

A , KaVo™ NOMAD Pro 2™ handheld x-ray unit. B , Proper operator position for handheld x-ray unit which maximizes operator protection from backscatter radiation. All operator body parts are within the shields protective range.
A, Courtesy KaVo, Charlotte, NC. USA; www.kavo.com
Because of their convenience and popularity, several handheld units are now commercially available. There is concern that some newer units do not have the same degree of protective operator shielding. This aspect is a critical feature when considering a handheld unit of choice.
Despite their convenience for remote venues, the units lack the power of the wall-mounted units. However, smaller power packs are necessary to keep the unit at an appropriate lighter weight for the handheld use of the typical office staff member. Hence, remote charging and reinserting battery packs become an additional maintenance task. Care must also be taken when lifting and handling the nonergonomic units to avoid shock damage.
Furthermore, there is concern that the features of portability do present challenges for optimal image quality and safety. Consequently, unless clinical facilities demonstrate distinct advantages of handheld units over wall-mounted units where the latter installations are possible, the routine practice of using handheld units over wall-mounted units is not always a recommended guideline.
Intraoral Image Receptors
As described in this chapter’s introduction, the types of sensors used in dental imaging have changed dramatically. Digital sensors are the preferred type of sensor for endodontic management. Although it has been shown that the digital image quality has no major advantages over film images, digital sensors are by far more practical than film. Digital sensors are advantageous in that there is reduced patient radiation exposure, with increased speed of image acquisition, storage, retrieval, and transmission. An additional advantage of digital sensors over film is that digital sensors forego the arduous chemical film processing, which takes longer and also requires the use of a darkroom. Digital sensors have dramatically facilitated the efficiency at which endodontic procedures can be completed.
Types of Digital Image Receptors
Digital image formats include indirect photostimulable phosphor (PSP) plates and the direct solid-state sensors that may either be the charge-coupled device (CCD) sensor or the complementary metal-oxide semiconductor (CMOS) active pixel sensor. The latter is also abbreviated as CMOS-APS.
Photostimulable Phosphor Plates
The PSPs are considered indirect because, after exposure, the sensor must be removed from the patient’s mouth and transferred to a laser scanner so that the stored latent electronic charges of the pixels on the sensor’s surface can be scanned with a laser light to generate an electrical signal. The digital process includes assigning a numerical value to the electrical signal strength of each of the pixels. These numerical values are then assigned a gray-scale value to be used by the imaging software for display on a monitor.
Solid-State (Direct) Sensors
The solid-state direct sensors transmit the electronic signal straight from the sensor directly to a computer so the image can be displayed in as little as 3 to 5 seconds or less, depending on the computer processing speed and the server’s size and efficiency.
At this time, the CMOS is the predominantly used direct sensor. They are generally less expensive to manufacture and are faster in transmitting the electronic signal for processing and require a simple USB connection to a computer. Despite the improved CCD sensitivity to x-radiation, their slightly greater manufacturing costs and their more cumbersome digital processing sequences have now decreased their commercial availability.
Despite the advantages and increased preference for direct digital sensors, there remain some disadvantages, which delay an industry-wide total conversion to these sensors. Direct digital sensors are thicker (5 to 8 mm) and less comfortable than the thinner and more flexible traditional film or PSPs. Because of this discomfort, not all patients tolerate imaging procedures with direct sensors. Although the direct digital sensors have the approximate height and width of conventional film sensors, the actual active sensor area is smaller, ranging among different manufacturers from 20% to 25% reduction of the image surface area compared with conventional film or PSPs. ,
This problem creates issues with cut-off apices from the compromised vertical dimension and missing apices when the horizontal dimension is compromised, and horizontal angulation is needed to image the multiple root apices of multirooted teeth.
Dental Film
For those clinicians still using dental film, “F”-speed film is the film recommended for endodontic use. However, the slower “D”-speed film is still available, the increased radiation exposure and slightly higher contrast are not of any added benefit for endodontic imaging. Although the active surface areas are larger on film (as previously discussed), this technology is being replaced by direct sensor technology. For clinicians still using dental film, a more detailed discussion of their use and chemical film processing is discussed in other reference sources.
Techniques for Intraoral Image Capture

Receptor Stabilizing Devices for Intraoral Imaging.
A , A hemostat is used for grasping film or a PSP plate and does help orient the x-ray beam. B , A hemostat holds a plastic holder for a solid-state digital sensor. C , The Rinn XCP-DS ORA receptor stabilizing-beam alignment device is used for standard periapical projections. D, The XCP-DS FIT Universal Sensor Holder and beam alignment device for working endodontic radiographs. This sensor holder stretches to fit all types of receptors including solid state sensors.
C, Courtesy Dentsply Sirona, York, PA; D, Courtesy Dentsply Sirona, York, PA
Due to the variability of human nature, it is not always possible to get patient cooperation to tolerate the placement of the instruments necessary for beam alignment. This difficulty is especially true for the “working” radiographs taken during an endodontic treatment with the rubber dam in place. Sometimes, it may require cooperation by the patient if they hold the sensor in position. In these scenarios, trying the modified paralleling technique is recommended . Essentially, the sensor is not parallel to the tooth, but the central beam is oriented at right angles to the receptor surface. In endodontic working radiographs, a further modification is made by varying the horizontal beam angle.
Tube Shift
Modification of the horizontal angle of the x-ray beam becomes a necessary modification to separate structures that superimpose one another on the 2D image. Principles of relative movement of structures and sensor orientation are applied to the differentiation of object position, as demonstrated in Figs. 3.4 and 3.5 .

A , The receptor is positioned parallel to the plane of the arch. The central ray (arrow) of the x-ray beam is directed toward the receptor at right angles. This is the basic beam–receptor relationship used for horizontal or vertical angulations. B , There is a clear outline of the first molar but limited information about superimposed structures (canals that lie in the buccolingual plane). The arrow points to a periodontal ligament space adjacent to a superimposed root bulge, not to a second canal.
From Walton RE: Endodontic radiographic techniques, Dent Radiogr Photogr 46(3):51–59, 1973.

These principles of tube shift have been adapted to object localization of structures in the nonvisible buccolingual dimension of 2D radiography. One of the most useful techniques in endodontics is the SLOB Rule. SLOB is an acronym― S ame L ingual O pposite B uccal, as first described by Richards.
When two objects and the sensor are in a fixed position buccal and lingual from each other, and the radiation source is moved in a horizontal or vertical direction, the images of the two objects move apart in opposite directions ( Fig. 3.6 ).

This schematic demonstrates the projected images of the blue circle (buccal) that is closest to the x-ray source and the red rectangle that is further from the x-ray source and closest to the receptor (lingual). In Position 2 of the x-ray beam, the objects superimpose on the Sensor 2 projected image. When the object superimposes on this single 2D image, it is not possible to tell which of the objects is positioned in the buccal or lingual position. When the beam is projected from Position 1 (i.e., left of Position 2), the objects are separated on the projected Sensor 1 image. The resulting image on Sensor 1 shows the red rectangle lingual object moved in the same left direction as the beam and the blue circle buccal object moved in the opposite direction of the beam to the right; hence, the acronym SLOB― S ame L ingual O pposite B uccal. When the beam is projected from Position 3 (i.e., right of Position 2), the objects are separated on the projected Sensor 3 image. The resulting image on Sensor 3 shows the red rectangle lingual object moved in the same right direction as the beam and the blue circle buccal object moved in the opposite direction of the beam to the left, hence the SLOB rule applies again.
Modified from: Abramovitch K. Imagery Chapter 5. In Impacted teeth , Alling III CC, Helfrick JF and Alling RD. WB Saunders, Philadelphia, 1993, pp. 110–116.
One way to visualize this effect is to close one eye and hold two fingers directly in front of the open eye so that one finger is superimposed on the other. By moving the head one way and then the other, the position of the fingers relative to each other shifts. The same effect is produced with two superimposed roots (the fingers) and the way in which they move relative to the radiation source (the eye) and the central beam (the line of sight). When the cone-shift technique is used, it is critical to know in which direction the shift was made and to determine what is buccal and what is lingual. Otherwise, serious errors may occur. Fig. 3.7 demonstrates how the horizontal angle is shifted to accomplish these localization techniques.

Horizontal angulation is determined by looking down from the top of the patient’s head. A, The position is set by aligning the horizontal plane of the position indicating device (PID) indicated by the arrow, parallel to the long axis of the hemostat handle. Mesial (B) and distal (C) horizontal angulations are then varied accordingly.
From Walton RE and Fouad AF, 2014.
This horizontal tube-shifting technique can be used to separate superimposed root canals and superimposed roots or to separate roots of teeth from adjacent superimposing anatomy, such as the mental foramen in the mandible or the zygomatic process of the maxilla in the maxillary arch. Examples of this tube shift are demonstrated in Fig. 3.11, A – F , of the next section.

A , The #14 palatal root apex is difficult to evaluate. B , By changing the horizontal angle by 20 degrees to the distal, the buccally positioned zygomatic process moves mesial (opposite the direction of the tube shift), and the palatal root can be evaluated better when isolated from the zygomatic process. C , Radiolucent area over the apex could be mistaken for pathosis. D , Pulp testing (vital response) and a more distal horizontal and increased vertical angulation show the radiolucency to be the buccal positioned mental foramen. With this distal angulation, the #29–#30 interproximal contact opens and the mental foramen moved more mesial and inferior to the #29 apex. E and F , The first premolar root outlines are not clear. By shifting the horizontal angle by 20 degrees to the distal, the outlines of the palatal and buccal roots are identified. The buccal root has moved mesially (opposite the direction of the tube shift), and the palatal root has moved distally (the same direction as the tube shift). Arrows point to the palatal and buccal apices.
Courtesy Dr. Jason Fowler, Loma Linda, CA.
Endodontic Imaging Needs

This standard periapical projection shows the root surface outlines with the periodontal ligament space and the adjacent lamina dura around the roots of the premolars and first molar. Even with the superimposition of the palatal and distobuccal roots, the root surface outlines (short, thick arrows) and the periodontal ligament space (longer, thick arrows) and adjacent lamina dura (long, thin arrows) still project, and the clinician must visualize these structures to evaluate periapical health.
The recognition of disease requires an understanding of the pulpal, periodontal, or periapical changes that may arise in the presence of disease and how these changes can affect the identification of the normal anatomic outlines. Similarly, an understanding of systemic or local hard tissue pathologic processes that affect the jaws is also necessary to recognize these processes as they present. The more astute clinicians recognize these changes in their earliest stages of tissue alteration. It is also important to remember that pathologic processes in their earliest stages are often symptomatic before the development of prominent radiographic signs or clinical signs or symptoms ( Fig. 3.9 ).

Only gold members can continue reading. Log In or Register to continue







